Pharma’s Future Depends on Patient Adherence
We look at an adherence toolbox, which allows patients and HCPs to achieve better results in the management of Ulcerative Colitis.

Ulcerative colitis (UC) is a long-term condition, where the colon and rectum become inflamed, causing symptoms like recurring diarrhea, abdominal pain, and a need to empty your bowels frequently. It’s a distressing condition, but treatments that effectively relieve symptoms and prevent them from recurring are available. The problem is, however, that patients are rather sloppy when it comes to taking their pills.
Studies have shown that non-adherence to medication is associated with a five-fold increase in risk of recurrence of symptoms, and yet, the rate of high adherence among UC patients is only 7%. “Adherence to medication is very important. Relapse has consequences for the individuals affected, but also for the carers and society,” said Mattias Norrman, Chief Operating Officer, Tillotts Pharma AG, a company that has recently launched a digital platform that aims to support patients with UC, called UCandMETM.
Project description
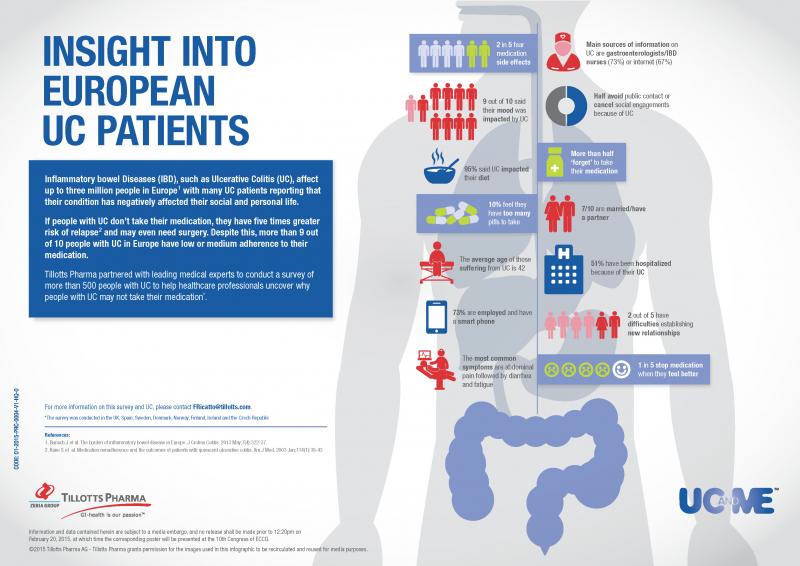
The platform was designed based on a survey of 507 patients across eight countries, which provided insight into patients’ needs and concerns. For example, the study revealed that 51% of patients forget to take their medication, while 20% stop taking their pills when their symptoms subside. “This is all with the knowledge that non-adherence increases the risk of relapse, and can even end in surgery. The consequences are potentially catastrophic, and yet people often neglect their treatment,” Norrman pointed out.
The same survey has shown that 19% of patients are afraid of side-effects, demonstrating the importance of effective communication between the patient and their healthcare provider. “There is a need to facilitate the way doctors and patients talk to each other. Nowadays, patients get a lot of their information from the internet, but that information isn’t always reliable, and often it’s too generic to apply to a particular patient specifically. It’s important to tailor the content to the specific needs and concerns,” Norrman said.
Doctors and nurses also provided their input into the design of UCandMETM. The platform, divided into space for patients and healthcare professionals, features a 10-item questionnaire collecting data on patient’s age at diagnosis, severity of symptoms, triggers, impact on mood, etc., which was created by the scientific board, and validated on 135 patients and 27 healthcare professionals. “This was designed to understand the needs of patients. The patient fills it out at the doctor’s office or before his or her visit. By using the answers from this questionnaire, the doctor can direct patients toward specific information that answers their individual concerns,” Norrman explained. After you have filled out the questionnaire, you’re provided with an individual patient code that you can share with your physician, who will provide you with relevant information.
On the healthcare professional side of the service, there are educational materials on diet, adherence, comments from other professionals like psychologists, recommended mobile adherence applications, etc. “What’s proven very useful are anatomical posters that can educate patients, which is much better than the sketches drawn by the doctor,” Norrman noted.
Those efforts culminated in an adherence toolbox, which allows patients and healthcare professionals to achieve better results in the management of UC available at www.ucandme.org. In the future, Norrman expects to expand the platform to several countries, making it available in a number of languages, with culture-sensitive content.
Customer response
Although the platform has only been launched a few weeks ago, the feedback has been very positive from both healthcare professionals and patients. “The most appreciated aspect of the project was its relevance. The questionnaire was easy to understand for the patient, but it was also informative. The one question most frequently asked at a doctor’s office is ‘Are you taking your medication?’. Patients invariably say yes, although it doesn’t reflect the reality. If you tweak the question, ask it slightly differently, you will have more insight into what is really going on. The bottom line is that you have to use short, time-efficient tools, so they can be adapted to individual patients.”
One of the biggest challenges with UC is that it’s a chronic, relapsing disease, associated with adherence problems. People stop taking their medication because they either forget, or start feeling better, or are afraid of the side-effects. Tools that allow doctors to communicate better with their patients, resulting in trust and mutual understanding, are essential as they have the potential to lead to better adherence. This, in turn, will likely end in better patient outcomes, which, at the end of the day, is all that matters.
http://www.sciencedirect.com/science/article/pii/S0002934302013839
http://www.nature.com/ajg/journal/v96/n10/abs/ajg2001726a.html