Understanding Patient Willingness to Pay
What steps should pharma and medical device companies take to ensure they get their pricing strategy right in self-pay markets?

A key feature of emerging markets is that patients often have to self-fund a high proportion of their healthcare costs. For all but the most severe conditions, public reimbursement of pharmaceutical products and personal medical devices is often partial to non-existent, particularly in the outpatient setting. While private health insurance coverage is increasing in many emerging markets, penetration typically remains low, even among middle to high income segments of the population. This means that for many drugs and devices, the primary means of purchasing in emerging markets will be patients paying out of pocket. Any successful pricing strategy therefore needs to start with an understanding of target patients’ willingness to pay for the drug / device in question.
In this article, I partner with Research Partnership Quantitative Director and pricing expert Duncan Munro to set out the critical success factors that should be considered in order to determine how a medical product should be priced in a self-pay market.
Understand the views all of the stakeholders who will influence the purchase decision
In any self-pay setting, the ultimate go/no-go decision to purchase a product is in the hands of the patient themselves (or their caregiver, in certain situations such as when the product is to be purchased for the very old, the very young or the very ill). However, other stakeholders also have a role in influencing this decision.
Physicians are usually the key gatekeepers as far as prescription products are concerned. A product that is strongly endorsed by physicians is more likely to command a higher patient willingness to pay than one that physicians are not convinced will offer their patients any real medical benefit. The doctor-patient relationship is also relevant, as when making prescribing decisions in cash-pay markets, financial considerations are inextricably intertwined with medical considerations.
Consciously or subconsciously, physicians often tailor their prescribing to the perceived income of the patient in front of them. For example, they may assume a particular patient is unable to afford an expensive drug, so they offer them a cheaper alternative. Therefore how physicians expect to prescribe a product, and their expectations around what price would be affordable for their patients, are important to understand when deciding how a prescription product should be priced.
In many emerging markets, the boundaries between ethical and over the counter pharmaceuticals are blurred. From Thailand to Colombia, ethical drugs can often be “unofficially” purchased from pharmacies without a prescription, despite repeated government attempts to regulate such practices. This means that pharmacists can be another influencer to consider when establishing patients’ willingness to pay, as they may exert control over purchase outcomes by recommending a specific brand or suggesting a cheaper alternative. However, pharmacists’ relevance varies across emerging markets; in China the majority of scripts are originated and filled in the hospital channel, with retail pharmacists having minimal involvement.
Realistically define the patient population with the potential to purchase the product
Once the views of other stakeholders/gatekeepers have been taken into account, the next step is defining the target patient population who are expected to be purchasing the product out of pocket. For example, while China has a population of 1.3 billion, around half of the population live in rural areas and have little access to any premium-priced medication; distribution channels are limited. Most forecasts are therefore based on the urban population of 600 million; for a particularly high-priced product, the forecast might be focused on just the tier 1 and tier 2 cities, in which patients have greater disposable incomes and access to better quality healthcare.
There are no fixed answers when deciding which patient population to consider for a particular drug or device as this is highly dependent on the product and the therapy area. Essentially, the same assumptions used to define the target market for forecasting purposes should be carried forward into the sampling for any market research conducted to understand patient price sensitivity. For example this might include only considering the views of urban patients whose household income is within the top ten percent of the country.
Explore all practicalities associated with using the product
Direct feedback needs to be obtained from a sample of relevant target patients regarding their willingness to pay for the product. This typically includes asking for both the self-stated price they would be willing to pay and their intent to purchase at prompted price points. While a range of techniques and question types of varying complexity can be used to explore this, to avoid overstatement it is fundamental to set up the scenario as realistically as possible, and make sure all relevant practical aspects of product use are communicated to the patient. Before giving their assessment of the price, patients need to understand as much about the product as possible. This is especially important if there is anything novel or unfamiliar about the product, or the administration is different from what they might be used to (e.g. oral vs inhaled). For example, if a patient already has a current device which would need to be replaced, the extent to which this would impact on purchase intent needs to be checked with the patient. Another element to explore with patients to anchor the scenario in reality is a consideration of what they would need to give up in order to pay for the drug.
The majority of medical purchases are not one-offs; repeat usage will likely also need to be considered when setting a price. There is an unavoidable uncertainty inherent in exploring how price will affect patients’ compliance and persistence, in the absence of the patient actually experiencing how the product works for them. However asking how many times patients estimate they would purchase the product over a fixed time period such as a year at a given price point can act as a proxy to help understand the extent to which price may dampen repeat demand.
For medical devices, there is often an additional layer of complexity involved in determining the optimum pricing because many devices include both a consumable and non-consumable part. Self-monitoring blood glucose (SMBG) devices for diabetes patients, which comprise of a re-usable meter and disposable test strips that need to be purchased on a regular basis, are a classic example. Price sensitivity to both the consumable and non-consumable parts of the device needs to be explored.
For pharmaceutical products, pack size is a relevant variable that may add complexity to any pricing scenario. Smaller pack size options may be more manageable for patients who have less available disposable income. “Sachet marketing”, or selling products in small amounts, has long been a common ‘bottom of the pyramid’ strategy to sell consumer good to low-income groups in emerging markets. For example in India over 80% of shampoo consumed is purchased in 0-50ml packs, in stark contrast to less than 5% in Western Europe, where 100ml + pack sizes dominate the market. If different pack sizes are being considered, or will be made available, patients’ price sensitivity to each option needs to be explored.
Determine the volume/revenue trade offs
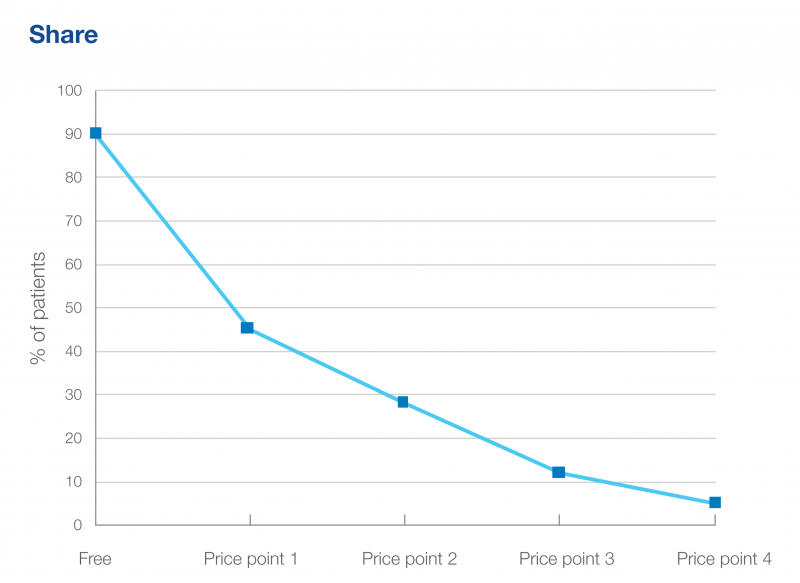
Price elasticity, the extent to which a higher price will lead to an increased or decreased revenue in a market, is a key output of willingness to pay research. Essentially this boils down to calculating whether more revenue will be generated from a small number of patients paying a large amount or a large number of patients paying a small amount. While a higher volume of patients will likely be open to purchasing the product at the lowest reasonable price, the revenue generated per individual purchase will be lower at this price. The extent to which increasing the price diminishes patient likelihood to purchase the product is therefore key information required to set a price that will maximise revenue.
There may however be good reasons not to operate in a lower-priced sphere. In medical devices, fixed costs of manufacturing can give less flexibility in pricing than pharmaceuticals, as a minimum price must be charged to cover these costs and make profit. It is also important to consider other external factors, such as how the price set in one market might impact the regional and potentially even global opportunity. If the product is being sold at a high price differential between neighbouring markets within a region, this leads to high potential for grey imports, which can damage a brand’s value.
There are other market-specific issues too: in India the government may grant compulsory licenses for drugs that it deems to be essential but too expensive for the Indian market, where most patients pay out of pocket. They first exercised this authority in 2012 with Bayer’s chemotherapy drug Nexavar, causing Bayer to lose out on direct sales in India by issuing a locally-based pharmaceutical company, Natco, with a licence to manufacture an affordable generic version.
Ultimately, setting the right price for a drug or device in any self-pay market involves striking the right balance between volume and revenue. To do this, it is critical to start with a solid understanding of stakeholders’ perceptions – both the patients themselves and the healthcare professionals who will influence them. When exploring these perceptions, care must be taken throughout to ensure the scenarios tested are realistic and that stakeholders fully understand what the product is offering. In this way, market research offers key insights into patient willingness to pay and provides an evidence based approach to price setting for novel products in self-pay markets.
Marc Yates is Director of Emerging Markets at Research Partnership and has 30 years’ experience of market research, specializing in healthcare research since 1996. He spent 15 years in Asia, originally based in Shanghai, then Hong Kong before moving to Singapore. In 2011 he relocated to London to take on a broader Emerging Markets role. Marc is a regular speaker at industry events and has presented papers on Emerging Markets at EphMRA and PBIRG conferences. Contact Marc at marcy@researchpartnership.com
Research Partnership is one of the largest independent healthcare market research and consulting agencies in the world. Trusted partner to the global pharmaceutical industry, we use our expertise and experience to deliver intelligent, tailor-made solutions. We provide strategic recommendations that go beyond research, helping our clients to answer their fundamental business challenges. Find out more at http://www.researchpartnership.com/



