Driving Earlier Diagnosis: A Case Study in Psoriatic Arthritis
Following a survey of 1000 Psoriatic Arthritis patients, Mary Assimakopoulos shares some of the root causes behind a late diagnosis of this debilitating illness, and the patients’ own feelings towards their standard of care.
In this month’s column we discuss how promoting earlier diagnosis of a chronic disease, such as Psoriatic Arthritis (PsA), should result in better patient outcomes and generate a larger treatment market.
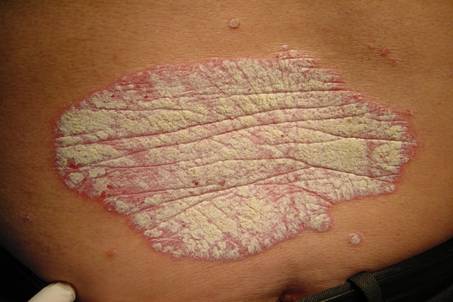
PsA is an auto-immune disease which causes inflammation of the joints, pain and stiffness, which is accompanied by patches of red and white, scaly skin indicative of Psoriasis.PsA gets progressively worse and can cause permanent damage to the joints. These worsening skin manifestations can have a severe impact on a patient’s quality of life, particularly if located in highly visible parts of the body. Almost a third of people with psoriasis will develop PsA but patients may experience arthritic symptomsbefore any skin manifestations. The exact causes of the disease are not yet known, but a number of genetic associations have been identified.
“It takes around 17 months from first experiencing symptoms to actually going to see a doctor and a further three years from the time a person visits their doctor to the time he or she is accurately diagnosed with PsA”
Because prolonged inflammation can lead to joint damage, early diagnosis and treatment is recommended and yet, in our patient research findings (carried out amongst people diagnosed with PsA across Europe), we have found that it takes around 17 months from first experiencing symptoms to actually going to see a doctor and a further three years from the time a person visits their doctor to the time he or she is accurately diagnosed with PsA. So in total the journey from awareness to diagnosis takes around four and half years, by which time, around 50% of patients feel that their disease has reached quite a severe stage1.
So what are the reasons for this protracted time that it takes for patients to be diagnosed with PsA? Firstly, PsA patients initially present with a wide range of symptoms ranging from skin disorders to articular or arthritic pain. 80% of PsA patients are initially diagnosed as having either a joint problem or psoriasis.1Is this due to the nature of how the disease initially manifests or are physicians still unclear on what signs to check for a full and complete diagnosis of PsA? It appears to be a combination of both.
Depending on the predominant symptoms, patients initially present either to their primary care physician, a dermatologist or a rheumatologist. All three physician types appear to often miss some of the diagnostic clues, which can result in an incomplete diagnosis (i.e. Psoriasis). Primary care physicians, in particular, are less aware of PsA diagnostic criteria and may delay referring a patient to a specialist for a significant period of time.
Complicating this further is the fact that symptoms can flare up and down, so although a patient may experience severe bouts of the disease, he may appear to have quite a mild and slowly progressing condition. In an interview with a patient from Italy we heard that “after 6 to 7 months of articular pain, I was referred to a rheumatologist, but as my symptoms came and went I decided not to see the specialist.”
Physicians need to regularly follow up their patients and be ready to re-evaluate their initial diagnosis. In particular they need to ensure that their examinations are comprehensive, as once patients are on a particular pathway, it can take much longer for the correct diagnosis to be made.
Patients are likely to benefit from being better informed about PsA and the possible implications that delaying diagnosis and treatment can have on their outcomes and long-term health. Our survey found that PsA patients feel that they didn’t get sufficient information from their physician at diagnosis. 62% said they were not offered adequate support, 47% said they weren’t given a full review of treatment options and 44% said they didn’t receive a full understanding of the impact of their PsA.
Unsurprising then, that many patients said they experienced quite negative feelings upon being diagnosed, with many saying they felt “uncertain”, “anxious”, “frustrated” and “afraid”. Could pharma do more with patients and with doctors to help allay patients’ fears and move them to a more positive emotional state? Certainly those patients who are on biologics such as Enbrel, Humira and Remicade, are more positive at initiation, describing themselves as “hopeful”, “cared for”, “optimistic”, “confident” and “informed”.
“Physicians should engage their patients in an open discussion about their disease, their objectives, expectations and treatment preferences”
However, 62% of patients on DMARDs said that their doctor had not even discussed the possibility of a biologic treatment with them – despite the fact that these treatments are far more effective at stopping disease progression. Whilst not all DMARD patients would be eligible for a biologic, could increasing patient awareness of these aggressive treatments lead to improved acceptance?
Our PsA Therapy Watch tracking survey based on more than 8,000 PsA patients from 5EU markets shows that only 39% of PsA patients are on a biologic2. There is evidence that primary care physicians and dermatologists are not as confident about initiating biologic treatment for PsA and it would be better for the PsA patient to be referred more quickly to a rheumatologist for earlier initiation on to a biologic, thus resulting in a better outcome.
There is certainly room to improve the quality of the physician / patient relationship. Physicians should engage their patients in an open discussion about their disease, their objectives, expectations and treatment preferences, in order to maximize compliance and adherence over time.
In conclusion, I believe there are a number of market shaping opportunities for pharma to improve awareness about PsA, its diagnosis, progression and optimal treatment options. This will result in improved patient outcomes as well as substantially increase the market opportunity for treatments.
1Living with Psoriatic Arthritis is an online patient survey conducted by the Research Partnership, and undertaken with 291 patients diagnosed with PsA in France, Germany, Italy, Spain and the UK in May-June 2012. In-depth follow-up interviews were conducted with 30 patients across all markets.
2PsA Therapy Watch tracking survey is based on 8569 PsA patient records collected across the 5EU markets from Jan – April 2013.

